Testimony before Congressional Oversight Committee on Autism and Immunization
Mr. Chairman and members of the committee:
This testimony represents the scientific findings of data accumulated over the past year and a half from autistic children during the course of standard evaluations of their gastrointestinal symptoms. This testimony should in no way be taken as anti-vaccine. Children in my pediatric practice continue to receive all vaccinations in accordance with the guidelines set forth by the American Academy of Pediatrics. The observations expressed herein are my own, and do not represent the opinions of any institution, organization, clinic, or medical practice with which I may be associated.
My
involvement with autistic children began approximately one and a half years ago. At that
time, I was approached by a colleague who was caring for a large number of autistic
patients. He observed that a large proportion of these patients suffered from chronic,
unexplained gastrointestinal symptoms and that these symptoms were a source of great
anxiety to the parents. I agreed to evaluate them, and my findings are detailed below. The
evaluations undertaken were standard “textbook” evaluations of children with
chronic diarrhea, constipation, and abdominal pain, uninfluenced by the fact that these
children were autistic.
Patient Population
Our
experience consists of a total of 43 consecutive children aged 2-10 years of age. Most
were referred by private practitioners but many were self referred after much frustration
with their children’s ongoing discomfort. 42 patients
had received a diagnosis of either autistic disorder or autistic spectrum disorder by a
pediatric neurologist or developmental pediatrician. Many children had received
independent confirmation from a second or even a third pediatric specialist. In no
instance was the diagnosis disputed by a second specialist. The remaining patient carried
a diagnosis of Aspergers syndrome.
The
majority of patients had a clear history of developmental regression. Specifically, these
children developed in an entirely normal fashion for the first 12-18 months. They
typically had a vocabulary of 15-25 words, maintained normal eye contact, were playful and
interactive, and were not overly irritable. At some point during this age interval of
12-18 months, they had either a precipitous or gradual decline in all the above mentioned
developmental markers, and this was accompanied by the appearance of typical autistic
behaviors, “stimming”, and bouts of unexplained irritability. In some patients,
verbal stagnation, but not regression occurred. However, in these patients, clear
regression was seen in the interactive and social skills of the children.
The
majority of patients are from the northeastern United States. The ratio of males to
females was 7:1.
Symptomatology
The
most common gastrointestinal symptom noted by the parents was diarrhea. In some children,
the diarrhea took the form of a soupy liquid that occurred 4 to 7 times per day and would
frequently leak from the child’s diaper. However, the majority of parents reported a
stool frequency of 1-3 per day with a consistency of mashed potatoes. The stool is
particularly malodorous, and usually contains pieces of undigested foods. Irritability is
often noted just prior to the bowel movement.
Constipation
is another frequent complaint, consisting of bowel movements every 3-6 days and typically
accompanied by great irritability upon passage of the stool. The consistency of the passed
stool was not overly hard, suggesting that these children are actually withholding stool
and not truly constipated in the strict sense of the term. This constipation is often
accompanied by abdominal distension and flatulence. Most patients experienced periods of
diarrhea alternating with periods of constipation.
Abdominal
pain is another frequent complaint. Most of these children are poorly communicative, and
parents often rely on body language cues in determining that their child is experiencing
abdominal pain. Children often drop unexpectedly to the floor howling and screaming. This
often lasts for up to half an hour. Many children clutch their abdomen and bend over. Some
assume a fetal position on the bed or floor, and others take the parents hand and rub
their abdomen.
Finally,
we have noticed that most regressive autistic children show poor growth, with the majority
falling in the lower 10th %tile weight for age. Interestingly, there does not
seem to be a concomitant percentile deficit in height for age.
Evaluation
All
children underwent initial evaluation of their gastrointestinal symptoms. This included a
thorough history and physical exam, complete blood count with platelets, erythrocyte
sedimentation rate, serum chemistries, celiac antibody panel with serum IgA, inflammatory
bowel disease serology, and stool examination for ova and parasites, culture, and occult
blood. The patients diet was thoroughly reviewed to assure that it did not contain
excessive nonabsorbed carbohydrates or fruit juices. Therapeutic alterations in the diet
were undertaken, including the removal of all gluten and casein containing foods.
Medications and supplements were reviewed to assure that they did not contribute to the
symptoms.
The evaluation above invariably did not lead to a diagnosis and patients then underwent colonoscopy. Upper endoscopy was performed only if pain was a predominant complaint or if celiac disease was strongly suspected.
Findings
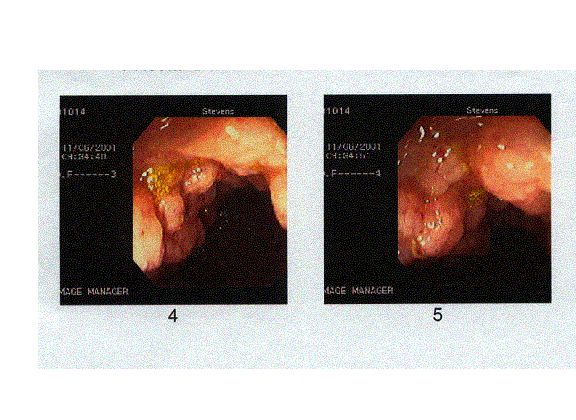
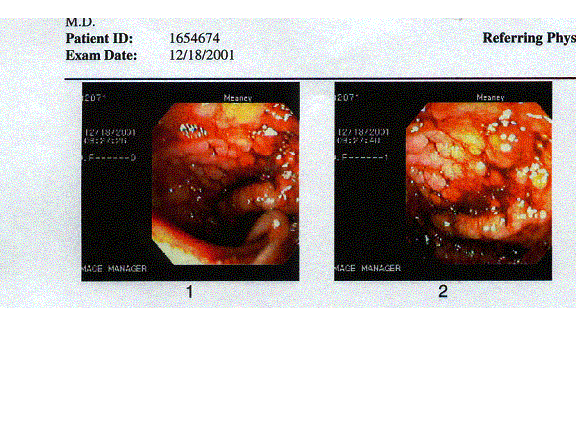
The
above images depict the terminal ileum in two patients. They are representative of the
gross endoscopic findings of 90% of these patients in whom the lymphoid nodules of the
terminal ileum were found to be markedly enlarged. This is in agreement with the
previously published findings of Dr. Wakefield in which a similar proportion of patients
were found to have abnormal lymphonodular hyperplasia of the terminal ileum.
The
second significant finding in our series was on histologic evaluation of the biopsy
specimens. The results are summarized below.
% patients with colitis |
28/43 |
65% |
% patients with active colitis |
22/43 |
51% |
% patients with chronic colitis |
17/43 |
40% |
% patients with eosinophilic colitis |
3/43 |
7% |
% LNH (macro) of terminal ileum |
36/40 |
90% |
% neither active, chronic, nor eosinophilic |
15/43 |
35% |
Colitis
was determined as per the report of the institutional pathologist. The interpretation of
whether the degree of inflammation represented true pathologic inflammation versus a
normal variant was subject to the personal experience of the individual pathologist and
was not subjected to a uniform rating system.
The
patterns of inflammation were patchy and unpredictable in any given patient, but overall
were noted in all parts of the colon and terminal ileum. Although the table above lists
chronic and active colitis separately, most patients with colitis had both chronic and
active inflammation. Most patients had at least 3-4 distinct areas of histologic
inflammation, with an equal number of biopsies that were histologically normal. The
intensity of the inflammatory lesions varied as well, with many being subtle and somewhat
focal, and others being more marked and diffuse. The latter included areas of cryptitis,
crypt abscess, ulcerations, and dense inflammatory infiltration. One patient was found to
have an inflammatory polyp. Most significantly, these findings were consistent and seen
repeatedly amongst the majority of patients.
In
regards to the last group of patients in the table above, it should be noted that although
the histology did not reveal pathologic colonic inflammation, the majority of these
patients were found to have a heavy and diffuse lymphoid hyperplasia of the colon
(macroscopic and microscopic), signifying an activation of the colon’s internal
immune system.
Conclusion
In
a series of 43 autistic children, mostly regressive, with chronic gastrointestinal
symptoms, the majority were found to have pathologic inflammation of the colon and
terminal ileum. 90% had pathologic lymphonodular hyperplasia of the terminal ileum.
Moreover, the findings were similar and consistent from patient to patient within the
affected group.
Questions
1)
Does autistic colitis occur equally in regressive vs. non-regressive autism?
2)
Do differences in growth exist between the colitis and non-colitis group?
3)
Do differences in growth exist between the regressive vs. non-regressive group?
4)
In a retrospective analysis of growth, will onset of growth failure coincide with
the onset of regressive behaviors?