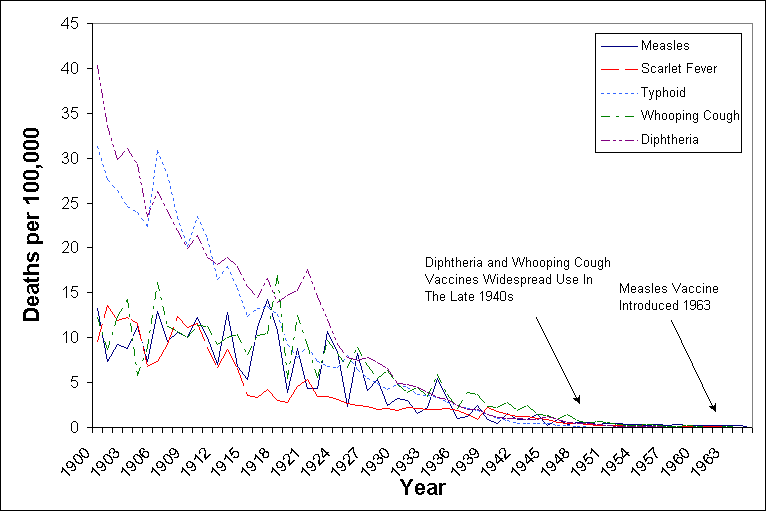
Figure 1. Death rates from infectious diseases
Vaccines
and Disease
An investigative Report
July 12, 2001
Updated: November 6, 2002
Updated: November 18, 2002
Roman Bystrianyk
The fatal tendency of
mankind to leave off thinking about a thing which is no longer doubtful is the
cause of half their errors.
– John Stuart Mill
|
I |
n 1949, the DTP vaccine was licensed to prevent diphtheria, tetanus, and pertussis (whooping cough) issuing forth the modern use of vaccines in the prevention of childhood illnesses. Polio immunization was later introduced to prevent that dread disease. In 1963, the measles vaccine was licensed and was combined with mumps and rubella vaccines to create the MMR vaccine. In more recent times the hepatitis B and chickenpox vaccines have been developed and incorporated into our healthcare system. Now a child can expect to receive up to 33 vaccines during their childhood with more vaccines on the horizon, such as herpes zoster (shingles), West Nile virus, influenza, pneumococcal, HIV, and many more.
The belief that vaccines are safe and effective is pervasive in today’s society. The vast majority of the medical, public, and government communities have a well-established belief system in the benefits of vaccines. Even children’s books show how important it is to “get a shot from the doctor to keep us well.” Our belief system is so ingrained that we look to medical science to create new vaccines to protect us from everything from AIDS to ear infections.
Unlike almost any other health-related issue in the free world, governments mandate many vaccines for the theoretical public good. In the United States, all 50 states require a large number of vaccinations before children are allowed to attend public schools or day care centers. Although most states have religious and medical exemptions, with some having a philosophical exemption, public and medical officials exert a great deal of pressure to vaccinate. The pervasive attitude that plagues will return and ravage the western world without everyone giving their child a full set of vaccinations is a powerful force in modern society.
One of the chief concepts that vaccine proponents tell us, and that we generally believe in modern society, is that the use of vaccines is responsible for the virtual elimination of many childhood scourges that used to ravage the world. We are told, and assume, that in the 1800s and early in the 1900s many diseases killed a large number of people, and that vaccines were invented and stopped these diseases from being a threat. But is this in fact the case? An immunization booklet produced by the CDC (Centers for Disease Control) states the following:
“Why are baby shots so important? These shots protect your baby from nine diseases: measles, mumps, rubella (German measles), diphtheria, tetanus, pertussis (whooping cough), polio, Haemophilus influenzae type b (Hib disease), and hepatitis B. Are these diseases very serious? Today we might not think of these diseases as being very serious because thanks to vaccines, we don’t see them as often as we used to. … Measles used to kill hundreds – sometimes thousands – of people a year. In the 1920s, over 10,000 people a year died from diphtheria.”
“Years ago, diphtheria was a widespread and greatly feared disease. Through the 1920s, it struck about 150,000 people a year and killed about 15,000 of them. Since then these figures have dipped considerably, thanks to parents who have gotten their children vaccinated against this terrible disease. There were only 918 cases in 1960, 435 in 1970 and 128 in 1976. Today, only a few cases occur each year.”
“Before measles vaccine was available, nearly all children had measles by the time they were 15 years old. An average of 530,000 cases a year were reported in the United States during the 10 years before vaccine was available. And during each of these years, over 450 people died because of measles. Now, thanks to the measles vaccine, the number of measles each year is a fraction of what it was then.”[1]
These statements are certainly compelling. On the face of it, we cannot help but assume that vaccines have played a key role in improving all of our lives. But looking carefully at the evidence over a longer period of time reveals a different picture of disease evolution and the role vaccines have played. One Swiss scientist that analyzed data over a longer period of time came to a different conclusion of what occurred in Switzerland:
“An analysis has been made of the evolution in Switzerland of mortality due to the main infectious diseases ever since the causes of death began to be registered. Mortality due to tuberculosis, diphtheria, scarlet fever, whooping cough, measles, typhoid, puerperal fever and infant gastro-enteritis started to fall long before the introduction of immunization and/or antibiotics. The decline was probably due to a great extent to various factors linked to the steady rise in the standard of living: qualitative and quantitative improvements in nutrition; better public and personal hygiene; better housing and working conditions and improvements in education.”[2]
In that research paper, several graphs of death rates in Switzerland show massive drops in deaths from disease long before vaccinations are introduced. One graph shows diphtheria death rates for children from 0 to 14 years of age peaking at over 200 deaths per 100,000 in the late 1800s. This is followed by death rates decreasing to less than 10 deaths per 100,000 near the time of the introduction of the vaccine in the mid 1930s. There was an apparent 95 percent decrease in diphtheria death rates before introduction of the vaccine. Another graph within the same study shows scarlet fever decreasing from 200 deaths per 100,000 in the late 1800s to virtually zero by the 1930s before drug treatments were introduced. Yet another graph in the study shows typhoid also decreasing from 50 deaths per 100,000 in 1876 to virtually zero by the 1940s when drug treatments were introduced.
A review of “Childhood’s Deadly Scourge” states:
“During the last two decades of the 19th century diphtheria was the leading cause of death of toddlers in the industrialized world, in some cities killing more than a thousand in a single year. In contrast, since 1980 fewer than 100 cases have been reported in the entire United States. Although diphtheria is hardly the only infectious disease to have thus faded, its story is unique because the early period of its decline can be directly linked to advances in bacteriologic knowledge and practice. Between 1880 and 1930 health authorities in New York City were responsible for much of the practical innovation in the control of diphtheria, as well as a good share of scientific progress.”[3]
The Vital Statistics of the United States contains compiled statistics for a wide variety of information since early in the 1900s. Among those are death rates from all diseases, including infectious diseases. An introductory statement from the 1937 statistics indicates that death rates from infectious diseases declined greatly in the early part of the century. These declines occurred well before the advent of vaccines to treat these conditions.
“The trend in death rates for specific causes, over the past 20 or 30 years, may be characterized by two general statements. In the first place, there has been a great reduction in the death rates for infectious and preventable diseases; in the second place, there has been an increase in the rates for certain diseases characteristic of older ages. Greatest proportional rate decreases have taken place for such diseases as typhoid and parathyroid fever, which has declined from a rate of 23.5 in 1910 to 2.1 in 1937; and diphtheria, which declined from a rate of 21.4 in 1910 to 2.0 in 1937. … The rate reductions for infectious and preventable diseases can be largely attributed to the development of modern public-health practice.”[4]
From these figures, we can see that death rates from typhoid decreased by 91% from 1910 to 1937 and death rates from diphtheria declined by 90.5% during the same time period. The decrease in diphtheria occurred well before the use of vaccination.
An even a more recent editorial statement from the Journal of Pediatrics states that proper sanitation was largely responsible for the early large declines in infectious diseases.
“… the largest historical decrease in morbidity and mortality caused by infectious disease was experienced not with the modern antibiotic and vaccine era, but after the introduction of clean water and effective sewer systems.”[5]
Again, in a 2001 paper in the Journal of Infection Control:
“The conquest of infectious disease and the health revolution it initiated is arguably one of the greatest achievements of Western civilization. Yet the phenomenon is largely unknown and rarely taught, even in history courses. Conventional wisdom usually assumes that conquest of infectious disease can be credited to well-known lifesaving innovations in medicine such as vaccines, antibiotics, and surgical asepsis. These icons are truly essential ingredients of modern medicine, and their contribution to human life and health in this century can never be minimized. However, except for the smallpox vaccination, which was introduced in 1798 and made compulsory in England in 1853, the overall contribution of medical innovations to the health revolution of the 1800s is difficult to validate. Diphtheria, tetanus, and pertussis vaccine arrived on the scene only after disease mortality rates already had been reduced significantly; measles, rubella, and polio vaccines did not become available until the middle of the 20th century, when most infant deaths were the result of other causes. The same holds true for sulfa drugs and antibiotics. Their contribution is unequivocal, but they did not affect mortality rates until the 1940s.” [6]
Another paper published in the premier medical journal The Lancet in 1977 by the Department of Community Medicine in the United Kingdom also indicates that vaccines were not responsible for the decline in disease rates in that country.
“There was a continuous decline [whooping cough deaths], equal in each sex, from 1937 onward. Vaccination, beginning on small scale in some places around 1948 and on a national scale in 1957, did not affect the rate of decline if it be assumed that one attack usually confers immunity, as in most major communicable diseases of childhood. … The steady decline of whooping cough between 1930 and 1957 is predictive of a linear exponential decay characteristic of a general and progressive lessening in the volume and spread of infection among the susceptible population. With this pattern well established before 1957, there is no evidence that vaccination played a major role in the decline in incidence and mortality in the trend of events.”[7]
The author’s conclusion that “there is no evidence that vaccination played a major role in the decline in incidence and mortality” is quite monumental and far different than the general public perception.
Thomas McKeown who was Professor of Social Medicine in the University of Birmingham Medical School between 1950 and 1978, is still regarded as a major social philosopher of medicine, and known for his important works on epidemiology and the practice and purpose of medicine. His conclusion was also that diseases were declining well before medical interventions such as vaccinations came into standard use.
“The distinguished epidemiologist Thomas McKeown (1912-1988) maintained that reductions in deaths associated with infectious diseases (air-, water-, and food-borne diseases) cannot have been brought about by medical advances, since such diseases were declining long before effective means were available to combat them.” [8]
Another author shows that disease and mortality was falling before the advent of vaccines or drug therapies:
“… in 1869 there were 716 deaths from typhus in London; by 1885 this had been reduced to 28; and at the beginning of the twentieth century there was none. Similar declines could be given for other infectious diseases. Tuberculosis began a remarkable disappearing act. Killing perhaps 500 out of every 100,000 Europeans in 1845, consumption slowly but continuously sank to 50 per 100,000 by 1950. Curative medicine played little part in that transition. The disappearance began before Koch discovered the tubercle bacillus. By the time antibiotics entered the picture, TB in cities such as New York had fallen to eleventh place in the death lists. And the mortality graphs for most of Europe’s fatal crowd diseases all dived before antibiotics had been marketed. Whooping cough killed 1400 children out of every million in 1850, but one hundred years later whooping deaths were less than 10 per million. Scarlet fever behaved in the same way. Measles, typhus, pneumonia, dysentery and polio all share similar histories. Their retreat had a dramatic impact on the European population. By 1900 civilization had lost its biological population check: infectious disease. After centuries of hostile encounters, humans and microbes found a new adjustment with little interference from drugs or vaccines. In some cases the microbe became less virulent (measles and diphtheria) or the human host more resistant (tuberculosis).” [9]
In the view of this, how can the statements made by the CDC on how “thanks to vaccines” diseases are a thing of the past be correct? Back in 1924 Mark Twain was quoted as saying, “There are three kinds of lies — lies, damned lies, and statistics.” When Mark Twain made this statement, his point was that numbers could be manipulated by the unscrupulous to misrepresent facts, to justify a particular bias, or fulfill a particular agenda. It is an unhappy fact of modern life that anyone with an idea can support that idea with statistics. The less the public knows about the source of the statistics, the more possible it is to have misinformation posing as scientific results.
Simple statements, such as “in the 1920s, over 10,000 people a year died from diphtheria”, although accurate are very misleading. Providing a piece of historical fact without any real context and mixing it with statements on how vaccines helped cure these diseases leads the reader to erroneously conclude that vaccines were instrumental in the massive declines of deaths from these diseases.
The CDC’s statements on vaccines only provide a few facts and then draw a conclusion on this limited information. To understand the role of vaccines, we must use the raw information and analyze it over a long period of time. The Vital Statistics of the United States provides the most accurate information of death rates from various causes starting early in the 1900s.[10] Figure 1 is a graph of the death rates from measles, typhoid, scarlet fever, whooping cough (pertussis), and diphtheria. Both the pertussis and diphtheria vaccines were made widely available in 1949 and the measles vaccine was introduced in 1963.

Figure 1.
Death rates from infectious diseases
This graph shows that large drops in disease death rates occurred long before vaccines were introduced. From 1900 to 1963, when the measles vaccine was introduced, death rates from measles had declined from 13.3 per 100,000 to 0.2 per 100,000 – a 98% decrease. From 1900 to 1949, death rates from whooping cough declined from 12.2 per 100,000 to 0.5 per 100,000 – a 96% decrease. From 1900 to 1949, death rates from diphtheria declined from 40.3 per 100,000 to 0.4 per 100,000 – a 99% decrease. These are clear and major changes in the severity of diseases well before any vaccines were introduced. Close up views (figures 2-4) of the diphtheria, pertussis, and measles death rates show this dramatic drop well before vaccination programs began.
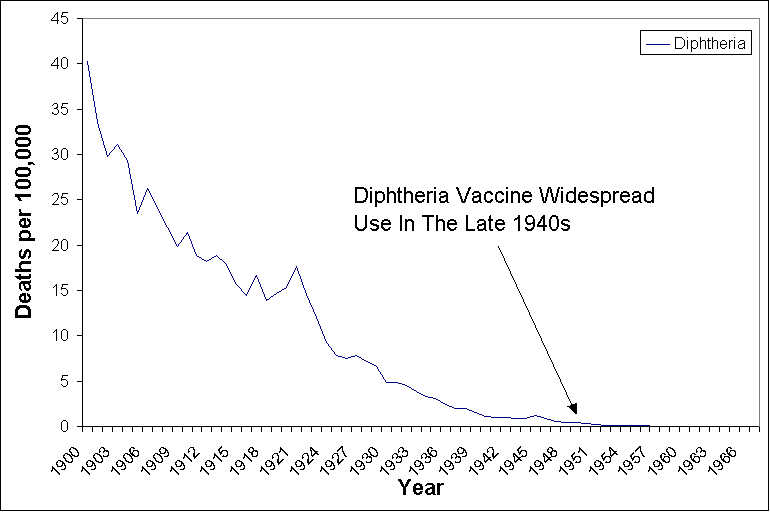
Figure 2.
Death rates from Diphtheria
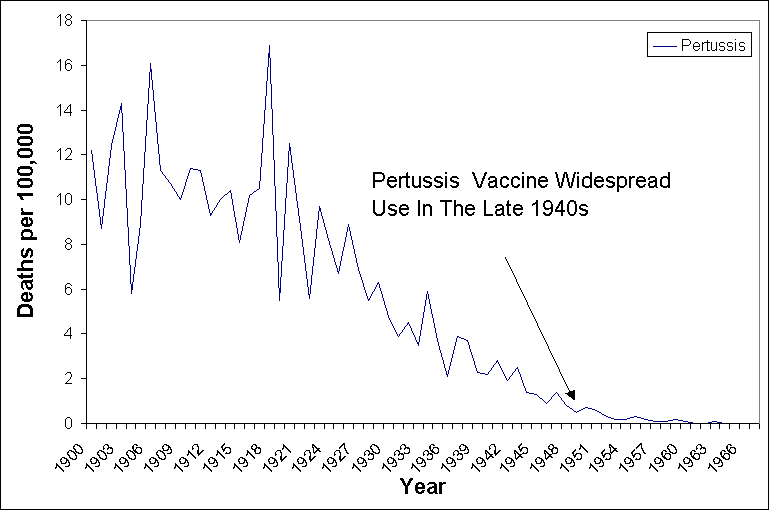
Figure 3.
Death rates from Pertussis
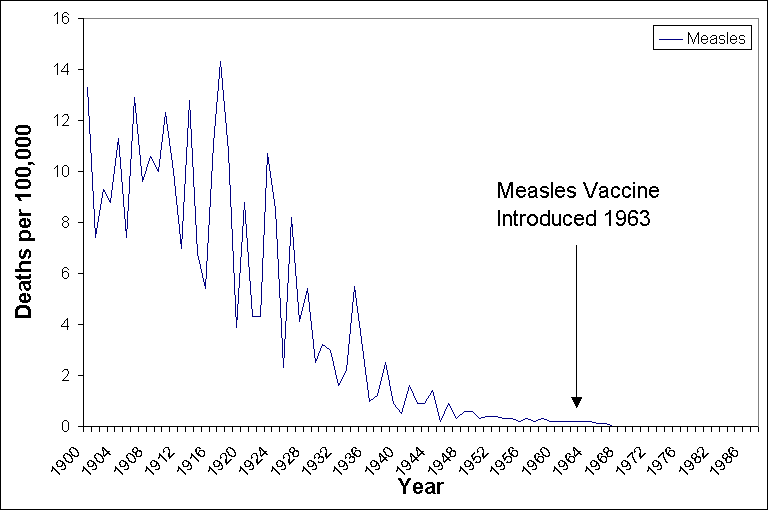
Figure 4.
Death rates from Measles
Similarly, in England and Wales we find the same decline in disease mortality. The data for the disease mortality was recorded 50 years earlier than in the United States, beginning in 1850. [11]
From 1850 to 1968, when the measles vaccine was introduced, death rates from measles had declined from a range of 52.11 to 26.6 per 100,000 to 0.11 per 100,000 – a range of 99.8% to 99.6% decrease. From 1860 to 1955, death rates from whooping cough declined from a range of 43.73 to 60.86 per 100,000 to 0.2 per 100,000 – a 99.5% to 99.7% decrease. From 1859 to 1940, death rates from diphtheria declined from a range of 49.2 to 22.7 per 100,000 to 6.77 to 1.83 per 100,000 – a 96.2% to 70.2% decrease. The exact decrease in mortality is difficult to obtain because the mortality from these diseases fluctuated from year to year, and the exact introduction of a vaccination and number of people vaccinated each year is difficult, if not impossible, to obtain. However, it is clear that death rates in England did to a large extent decline before vaccinations were widespread.
Figure 5 is a graph that shows the mortality rate declines in England and Wales. The gap from 1891 to 1900 is because data was not acquired for those specific dates.
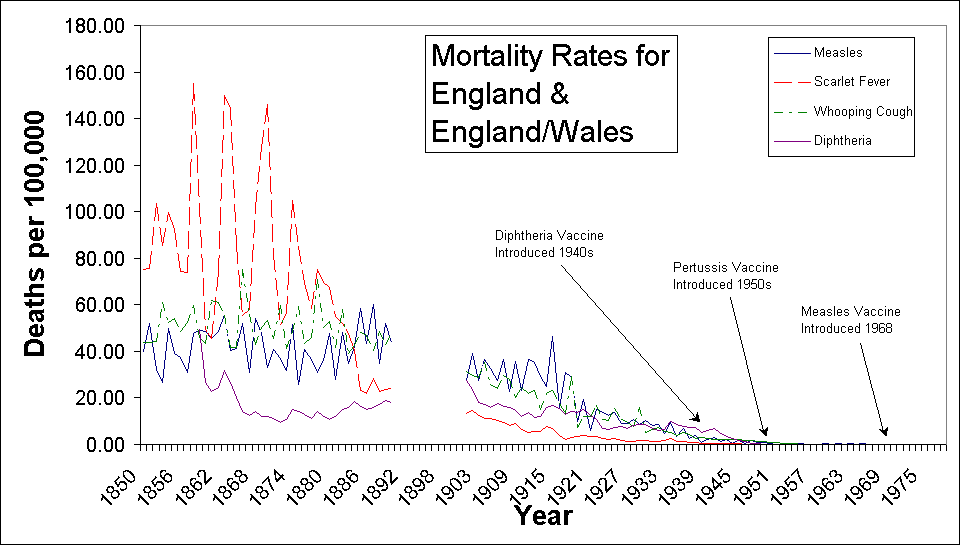
Figure 5.
Death rates from infectious diseases in England and Wales
The modern era of vaccines actually began with the advent of the vaccine against smallpox. Edward Jenner was aware of the belief that people who contracted cowpox never contracted smallpox. He hypothesized that inoculating people with cowpox would immunize them against smallpox. On May 14, 1796, he inoculated an eight-year-old boy, named James Phipps, with matter taken from a cowpox pustule. Phipps developed coxpox and quickly recovered. Several weeks later, Phipps was inoculated with smallpox and did not contract the disease. In 1798, Jenner reported his work in the book, “An Inquiry into the Causes and Effects of the Variolae Vaccine.” This book prompted the medical professionals of the time to adopt the practice of vaccination. The vaccine was introduced in England in 1798. It was later made compulsory in 1853 through the Compulsory Vaccination Act, and then in 1867, an even more stringent law was passed to enforce vaccination.
Looking at the raw data
from England during that era
[12],
as shown in Figure 6, we see that despite enforced vaccinations against
smallpox there was no significant decrease in deaths from smallpox. In fact,
three major epidemics during 1857-1859, 1863-1865, and 1871-1872 occurred, even
though there was a high vaccination rate. The last major epidemic in 1871-1872
had death rates of 101.2 and 82.1 per 100,000 people respectively, occurring
just four years after a newer and more strict vaccination law was enacted in
1867.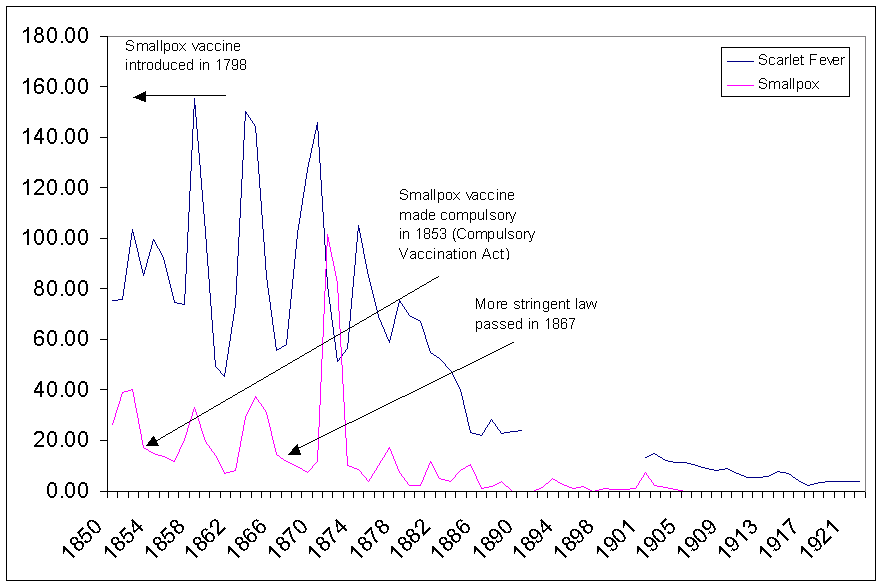
Figure 6. Death rates from smallpox and scarlet fever in England.
Another interesting point is that the smallpox disease cycle of decreased deaths and epidemics appears closely tied to the scarlet fever disease cycle. Just as there was a large decrease in scarlet fever deaths after 1885, there was simultaneously a decrease in smallpox deaths. It is important to remember that death from scarlet fever, which was the worst of infectious diseases in that era, was eliminated without any vaccination program.
Figure 7
shows that vaccination coverage had no apparent affect on smallpox deaths. As
coverage fell to from a high of 86% in 1879 to 61% in 1898 there was no
resurgence of smallpox deaths. There was a small increase in smallpox deaths to
7.5 per 100,000 people as vaccine coverage rates again increased to 71.8% in
1902, but there after, as vaccine rates fell to below 40%, there was no increase
in smallpox deaths. In fact, after 1905, deaths from smallpox almost completely
vanished.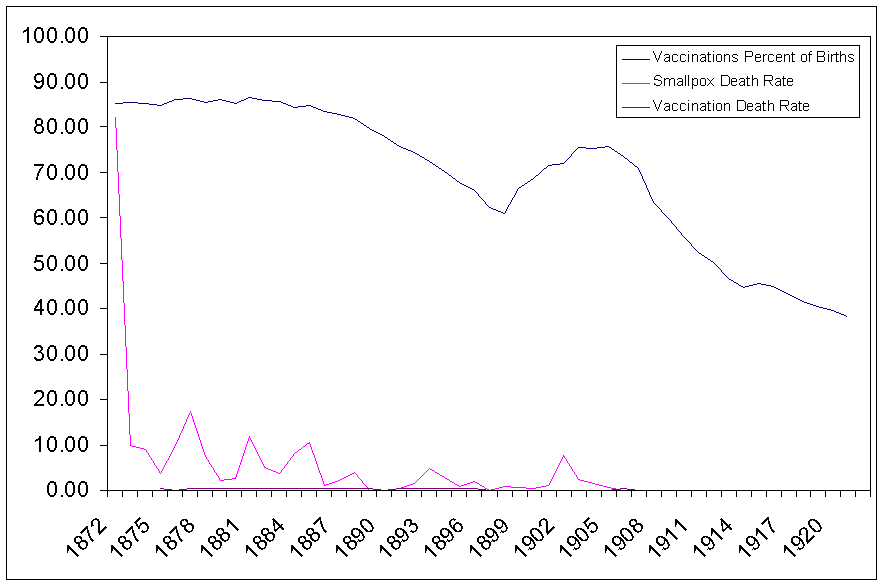
Figure
7.
Smallpox deaths and vaccination percent of births.
We must also remember that
deaths were directly attributable to the smallpox vaccine. Figure 8 shows the deaths per 100,000 that were caused by the
smallpox vaccine. Although the number of people that died from the vaccine is
small compared to the number of people that were killed directly by smallpox,
after 1888 there were years that the deaths from the vaccine was close to or
exceeded that from the disease itself (e.g. 1889 – smallpox: 23, vaccine: 58;
1890 – smallpox: 16, vaccine: 43; 1891 – smallpox: 49, vaccine: 43). After
1905, as can be seen in Figure 9, the number of deaths from smallpox and vaccination were very
close to one another. In point of fact, after 1905, a person was almost as
likely to die from the vaccine for smallpox as from the disease itself.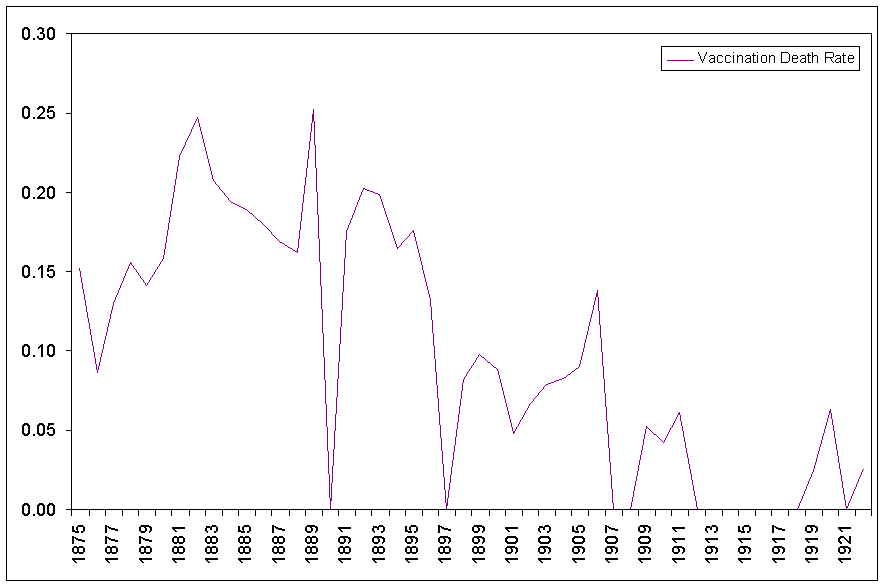
Figure
8. Deaths
per 100,000 from cowpox and other effects of vaccination
.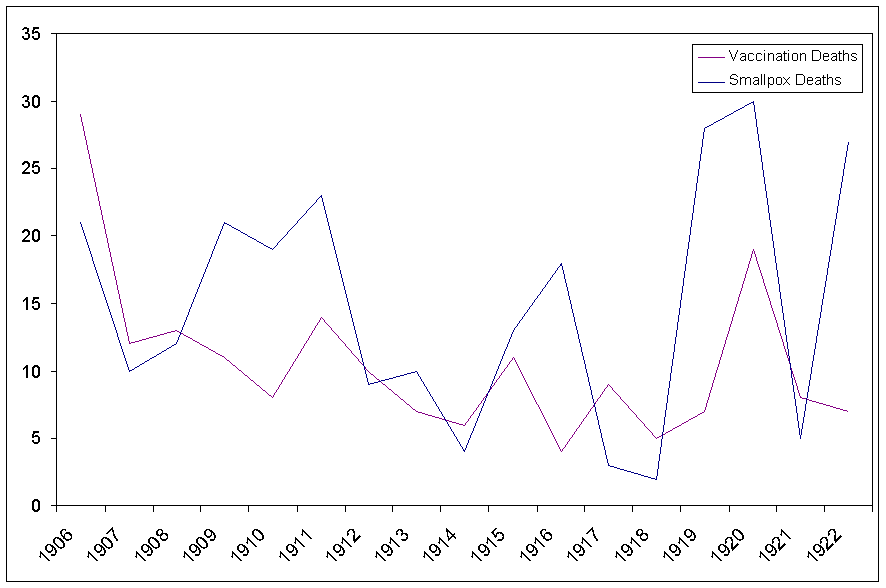
Figure
9. Actual
smallpox and smallpox vaccination deaths.
Another interesting point of note is that certain diseases that also once killed many people declined and vanished without any assistance from mass vaccination programs. Typhoid death rates of 10s per 100,000 each year was not uncommon. Scarlet fever once killed large numbers of people at a death rate of 100 or more per 100,000 each year. While quite deadly during their prime, these two “killers” were in effect eradicated due in large part to advances in hygiene and a better understanding of germ activity. The Canadian Medical Journal contains the following statements in an advisory statement:
“Typhoid fever is caused by Salmonella typhi, which affects only humans, often causing serious systemic illness. The organism is generally transmitted by the feces or urine of the people with the disease or those who are the S. typhi carriers. The death rate is approximately 16% for untreated cases and 1% for those given appropriate antibiotic therapy. … The incidence of typhoid fever is very low in all of the industrialized countries. Approximately 70 cases are reported in Canada and 190 in the United States annually. The low incidence of typhoid fever in these countries is attributable to improved living conditions, better drinking-water quality and the treatment of sewage. The vaccine does not seem to play an important role in maintaining this lower incidence. Most infections occurring in the industrialized countries are acquired elsewhere. … It is certain that vaccination does not afford adequate protection when heavily contaminated foods are ingested. … There cannot be too much emphasis placed on hygiene and food precautions; these measures appear to be the most effective protection against the disease.”[13]
If the forces of improved living conditions, better drinking water quality and the treatment of sewage virtually eliminated illnesses such as typhoid and scarlet fever, then isn’t it reasonable to consider that other diseases, such as measles and pertussis, would have had similar fates? An analysis of the death rates for all these diseases does support this idea. The Conquest of Disease by Thurman B. Rice, MD from 1932 states:
“The benefit of pure water is expressed not only by the lowering of the typhoid rate but also in a considerable lowering of other death rates, and even of the general death rate. … Why has the death rate [for Scarlet fever] markedly fallen in the days before the cause of the disease was understood? It must be remembered that a given germ is only part of the cause of a disease; there are often many other very important contributing, predisposing, or determining factors. As housing conditions were improved, as the general laws of sanitation, ventilation, and personal hygiene came to be better understood; as we came to insist on individual drinking cups; fresh air in bedrooms, and frequent bathing; as doctors became more proficient in treating the infection so as to prevent its serious complications and sequelae; as boards of health became more efficient in the enforcement of public health laws; as methods of isolation and disinfection were better understood the death rate declined accordingly.”[14]
Again, the major decline in mortality rates can be attributed to improvements in proper hygiene, not only at a societal structural level, but also due to major changes in attitude in personal hygiene.
“In addition to the seminal and recognized role of environmental hygiene, a substantial but overlooked component of the health revolution was the transformation in personal hygiene practices and cleanliness. The transformation probably started in the early 1800s, became extremely popular from 1890 to 1915, and has since become an essential feature of “civilized” behavior in the United States and Europe. It is proposed that this mass behavioral changes in washing, bathing, laundering, and domestic hygiene practices contributed significantly to the continuing reduction of illness and death rates at the beginning of the 20th century.” [15]
It would appear that, at best, vaccines could be credited with only a tiny fraction of the overall decline of disease deaths in the 1800s and 1900s. Because death rates were declining, it is impossible to say whether vaccines had a real effect or if that the same forces that caused the majority of the decline would have continued to have a positive impact. Those forces were primarily that of improved sanitation, proper personal hygiene, improved diet, and the natural cycles of disease.
Based on our knowledge that proper sanitation, improved living conditions, and improved nutrition were the key factors that caused declines in these diseases, we can ask the question: are the present deaths and complications from these diseases in people of poor socioeconomic or compromised nutritional status? Is it possible that the focus on mass vaccination programs diverted attention from continued improvements in sanitation and nutrition that could have further reduced or eliminated disease deaths and complications?
It would seem that the people who recognized the underlying cause of diseases and instituted better living conditions, proper water and better sanitation should be recognized for their remarkable achievements, not the inventors and promoters of vaccines. This analysis, which is based on historical and scientific studies, is a far different picture than the one alluded to by the CDC in their vaccine literature.
Because the focus has predominantly been on medical intervention, the history of what really caused the decline in disease mortality is “largely unknown” and “rarely taught”. The information that disease death declined before vaccination is important in the present day because we need to pay attention to these underlying causes of infectious disease. We must be ever vigilant to avoid returning to those disease-causing conditions and to examine these conditions when disease outbreaks occur. It is an important lesson in how we should approach disease prevention in third world countries. We should not forget the words of George Santayana: "Those who cannot remember the past are condemned to repeat it."
[1] Parent’s Guide to Childhood Immunization. U.S. Department of Health and Human Services, Public Health Service, Centers for Disease Control and Prevention, National Immunization Program, Atlanta Georgia 30333, 1993, pp. 1, 7, 21
[2] Gubéran, E., “Tendances de la mortalité en Suisse”, Schweiz. Med Wschr. 110, 1980, pp. 574-583
[3] Morman, E.T., “Childhood’s Deadly Scourge: The Campaign to Control Diphtheria in New York City, 1880-1930”, The Journal of the American Medical Association, April 12, 2000 Vol. 283, p. 1889
[4] Vital Statistics of the United States 1937 Part I, U.S. Department of the Census, 1939, p. 11
[5] “Zinc, diarrhea, and pneumonia (editorial)”, The Journal of Pediatrics, December 1999, Vol. 135, No. 6, p. 663
[6] Greene, Velvl W., PhD, MPH, “Personal hygiene and life expectancy improvements since 1850: Historic and epidemiologic associations”, American Journal of Infection Control (AJIC), August 2001, Vol. 29, No. 4, pp. 203-206
[7] Steward, Gordon T., “Vaccination Against Whooping-Cough Efficacy Versus Risks”, The Lancet, January 29, 1977, pp. 234-237
[8] Porter, Roy, “The Greatest Benefit to Mankind”, Harper Collins Publishers, 1997, p. 426
[9] Porter, Roy, “The Greatest Benefit to Mankind”, Harper Collins Publishers, 1997, p. 427
[10] Vital Statistics of the United States 1937 Part I, U.S. Bureau of the Census, 1939, pp. 11-12; Vital Statistics of the United States 1938 Part I, U.S. Bureau of the Census, 1940, p. 12; Vital Statistics of the United States 1943 Part I, U.S. Bureau of the Census, 1945; Vital Statistics of the United States 1944 Part I, U.S. Bureau of the Census, 1946, p XXII-XXIII; Vital Statistics of the United States 1949 Part I, U.S. Public Health Service, 1951, p. XLIV; Vital Statistics of the United States 1960 Volume II – Mortality Part A, U.S. Department of Health, Education, and Welfare, 1963, p. 1-25; Vital Statistics of the United States 1967 Volume II – Mortality Part A, U.S. Department of Health, Education, and Welfare, 1969, p. 1-7; Vital Statistics of the United States 1976 Volume II – Mortality Part A, U.S. Department of Health and Human Services, 1980, p. 1-7; Vital Statistics of the United States 1987 Volume II – Mortality Part A, U.S. Department of Health and Human Services, 1990, p. 11; Vital Statistics of the United States 1992 Volume II – Mortality Part A, U.S. Department of Health and Human Services, 1996, p. 12; Historical Statistics of the United States – Colonial Times to 1970 Part 1, Bureau of the Census, p. 58
[11] Mortality in England and Wales for 95 years as provided by the Office of National Statistics - Published 1997;
[12] Written answer by Lord E. Percy to Parliamentary question addressed by Mr. March, M.P., to the Minister to Health on July 16th, 1923
[13] “Statement on overseas travelers and typhoid fever”, Canadian Medical Association Journal, 1994, 151, pp. 989-990
[14] Rice, Thurman, A.M., MD The Conquest of Disease, The Macmillan Company, 1932, pp. 68, 121-122
[15] Greene, American Journal of Infection Control (AJIC), August 2001, Vol. 29, No. 4, pp. 203-206