Diphtheria
by Hilary Butler
HISTORY OF
DIPHTHERIA INFECTIONS AND DIAGNOSIS.
DECLINE OF DIPHTHERIA
IN DEVELOPED COUNTRIES
DISEASE PROCESS:
TREATMENT OF
DIPHTHERIA – NOW AND IN HISTORY
ALTERNATIVE TREATMENTS:
HOMOEOPATHY
HERBS
Diphtheria, like whooping cough and tetanus, is classed as a toxin-mediated disease. But diphtheria is better paired with scarlet fever, because both clinical syndromes are determined not by the bacteria, but by a class of virus called a B phage. This virus holds the genetic "key" to the production of the toxin that causes the classical membrane and neurological damage. Without this B phage, the diphtheroid family causes only minor, nuisance-value problems.
There are many different forms of non-toxin-producing, interrelated, relatively harmless "diphtheroids" that live with lots of other so-called disease-causing bacteria in our throats, on our skin, or in the environment. Most people would be horrified if they were told what could be cultured off a normal throat swab. Diphtheroids do not normally appear on most throat cultures because the normal culture medium for throat swabs is hostile to diphtheroids. If there is suspicion that diphtheria is a problem, then a special medium, which restricts the growth of all other bacteria, is prepared.
Many different species of Corynebacterium are widely distributed in nature and are commonly found in soil and water as well as on the skin and mucous membranes of humans and animals. Diptheroids are relatively resistant to adverse environmental influences such as dryness. They may survive for many weeks in dust and on dry fomites (books, toys, pencils, etc). The dust in hospitals and institutions may become heavily infected with dried pulverised secretions. Sources of infection are most commonly nose carriers, children with diseased tonsils, discharging ears or skin lesions. The infection is probably spread by airborne infected dust, contact with fingers, eating utensils or fomites and, possibly, by secretion droplets or droplet-nuclei.
Common environmental factors throughout history which have greatly increased the incidence and severity of diphtheria are shown in the following quotes:
"There is no doubt that exposure to sewage emanation is a fruitful source of diphtheria...the statistics of the association between the two are very positive." (Quain 1894, in Beddow-Bayly, 1939, p.105).
"…shows in interesting and conclusive fashion the definitive effect of school buildings, their construction and sanitation, on the spread of diphtheria. The highest incidence was observed in those schools where sanitation is most deficient and ventilation and lighting the least satisfactory. The brightest and airiest school showed the lowest incidence, and the incidence throughout all the schools placed them in exact order of sanitary virtue. Moreover, the incidence indicated the schools where malnutrition in the children is most conspicuous." (Medical World, 1931, p. 627.)
Even in America, there were those who recognised the lessons of the decrease of diphtheria prior to the use of a vaccine by saying:
"The eradication of diphtheria will not come through the serum treatment of patients, by the immunization of the well, or through the accurate clinical and laboratory diagnosis of the case and the carrier followed by quarantine; rather it will be attained through the mass sanitary protection of the populace subconsciously practised by the people at all times." (JAMA, 1922, p. 682.)
With regard to diphtheria in New Zealand, it is interesting in the light of the recent Auckland case, to note that during the period 1879 – 85, diphtheria in the Christchurch area was particularly severe. The majority of cases occurred in areas where there were either no sewers, or where the sewerage systems had grave sanitary defects. The water supplies were heavily contaminated, and the living conditions were beyond description. (Maclean, 1964).
Why is the issue of sewage important? There are many historical instances of sewage being relevant to the spread of disease, but even today very few textbooks mention this. A few days before the recent Auckland case, storm water had flooded the sewer system, resulting in raw sewage flowing onto the property of the family concerned. The Public Health Authority refused to investigate this potential causal factor. It could well be that the case had nothing to do with the parents' holiday in Bali, and everything to do with the presence of diphtheria from North Shore carriers in the sewage. Two years ago the Americans discovered that toxicogenic diphtheria has had continual undetected circulation for decades throughout areas in the United States and Canada. It remained undetected because they never looked for it, assuming it was eradicated. The same situation could quite likely exist here.
The recent Russian epidemic was caused, we were told, by low levels of childhood immunity (WHO, July 1993). But the majority of cases were in adults who had gone through a compulsory vaccination system that mandated 5 injections of diphtheria vaccine. According to the old philosophy, these people should have been immune for life. They now realise that immunity to disease requires 2 things: repeat exposure to antigen, and a healthy, stress-free body.Why do they say the epidemic was caused by inadequate childhood vaccination? By 1993, the situation was quite different and diphtheria is only now significantly reduced.
"Reported nationwide coverage among children aged 12-23 months increased from 72.6% in 1992 to 79.2% in 1993. During 1992-1993 at least 90% of children <5 years had received a primary series with diphtheria and tetanus toxoids and pertussis vaccine (DTP), or pediatric (DTY) or adult (Td) formulation diphtheria and tetanus toxoids, and approximately 80%, had received at least one booster." (MMWR, 1995, pg. 178).
Immunisation in Russia in the communist era was compulsory for children, with contraindications determined by the medical profession, not the parents. With ‘perestroika’ and choice, there was the start of anti-vaccine movement, led, ironically, by doctors not laypeople, which contributed to a slight fall in the vaccination levels. But these levels were still higher than those reported for the USA in 1990 and for Australia in 1995.
In the USA, they are at last admitting that there are several other factors involved in the Russian diphtheria epidemic. This is because high level transmission between adults was demonstrated in groups characterized by overcrowding, low hygiene levels, and high contact rates e.g.: the homeless and patients in neuropsychiatric hospitals (Vitek and Wharton). One important factor conducive to increased bacterial transmission was the deficient or lacking public health facilities, including routine access to functioning faucets for hand washing.
The other group looked at was the military, because 1.4% of Russia is armed. Recruits (who have already had 5 vaccinations – 3 primary doses, a 4th at about 2 yrs, and a 5th at 6 yrs; after 1980 Td was given at 11 yrs of age) were not revaccinated against diphtheria until 1990. Following outbreaks of diphtheria spread by the military in Kovrov District in 1983 and 1987, investigations in military units in various parts of Russia found carrier rates of toxigenic diptheria of up to 5.0%. There is nothing unusual about high rates of disease in military establishments. Extensive reading of military medical literature reveals some fairly callous reports about the necessity for toughening up recruits so that they have immunity to everything, and in the event of real stress, real war, they are unlikely to succumb.
In reality the majority of diphtheria in Russia has occurred in specific sub-groups. Refugees or persons displaced by internal conflict, the homeless, alcoholics, the military, and people living hand to mouth attempting to feed children. A very high proportion of cases were in women, a factor not well understood by the medical fraternity, but self-evident to those with common sense. Women (mothers) will feed the rest of the family before themselves. Interestingly though, one study reports that the death rate has been excessive in only one group – that of alcoholics. Their death rate was 25.7%, compared with the death rate of "normal" Russians of around 1%, despite the stresses associated with life in Russia.
It is also notable that the authors of this study said:
"We feel that a wide diphtheria epidemic in an industrialised country would probably not any more carry the high 10% mortality that it did in Europe and in the United States in the 1950's and 1960's". (Scand. J. Infect. Dis., 1996,p 41–46.
HISTORY OF DIPHTHERIA INFECTIONS AND DIAGNOSIS.
"Until we reach the beginning of the nineteenth century it is practically impossible to diagnose the nature of the various throat infections which are mentioned in medical writings. The great majority of them were probably of streptococcal nature, including typical scarlet fever and all the various forms of tonsillitis and quinsy. Children certainly died of "croup", a general term for any form of obstruction to breathing." (Burnet, 1972, p.193).
In the Appendices to Parliamentary Journals (Public Health Reports), all deaths from diphtheria in the earlier days included all forms of croup. In early New Zealand writings you can find quotes regarding the fact that some areas reported croup separately. For instance, Dr Nedwill's report to the Christchurch Local Board of Health stated:
"In Christchurch nine deaths occurred among 65 reported cases, but in addition to these deaths five others were referred to so-called "croup". It is unfortunate that this name is still retained as it includes two very distinct diseases – one of them a purely spasmodic origin, not very dangerous, and not infectious, the other true diphtheria." (Nedwill 1883, in Maclean 1964, p. 350).
Not long after this time, all croup, regardless of its nature, was included as a diphtheria death in New Zealand statistics, up until the vaccine was introduced. Nowadays, croup is considered to be caused by viruses belonging to the parainfluenza group.
"Early last century definite epidemics of what would today be called diphtheria occurred on the Continent, especially in France, Norway and Denmark. The disease was given its current name by Bretonneau in1826, but no more than a few stray cases were recognised in England until 1858, when there was a sudden widespread appearance of severe diphtheria in England, and within the year it had spread to almost every part of the globe.
It reached Australia, with the first case in Victoria in October 1859. The small isolated settlement in Western Australia remained free from diphtheria until 1864, when numerous cases occurred." (Burnet, 1972, p. 193-194).
In New Zealand, the highest year of incidence was 1874, with a total of 270 deaths, the highest ever on record (Maclean, 1964, p. 346).
"Wherever it appeared at this time, diphtheria was recognised as something outside the previous experience of physicians. The spreading grey membrane on the throat, the high fatality and the common appearance of paralysis of the muscles of the palate some time after infection were all new. Nevertheless, diphtheria in 1858 behaved epidemiologically like an infection that had long been present in the communities of the Western world. From the beginning it was a disease of childhood, not of adult life. Even before diphtheria appeared in its classical form, children must have been developing immunity against the responsible microorganisms and in 1858, those over ten years of age were nearly all possessed of sufficient immunity to avoid infection." (Burnet, 1972, p. 194).
Since 1858 typical diphtheria has been present in all the civilised communities of temperate climates. Its incidence and severity have shown the inevitable ups and downs. There was a second period of high mortality in Europe around 1880, then a steady fall for about thirty years until World War I with its drop in living standards and nutrition, and associated stress. Although the huge increase in diphtheria at this time was overshadowed by the influenza pandemic, epidemiologists noted a large increase in all infectious diseases. In Europe, the living conditions following World War I saw to it that diphtheria remained at quite high levels until around 1931, when the level started to fall. During World War II diphtheria became the most prevalent infectious disease in Western Europe, and the most common infectious disease contracted by American servicemen despite extensive immunisation being practiced (Biol. and Clin. Basis of Infect. Dis., 1985, pg. 230).
But by this time another trend had become apparent. Whereas at the start of the twentieth century only 1–2.5% of diphtheria cases were in adults, by 1938 that percentage had rise to 12%, and by 1943, 48% of cases were in adults. A similar trend was noted in New Zealand. By 1930, 22% of diphtheria was occurring in the 15+ age group, and by 1951, that proportion was 50%. Around this time too, a first in medical history, secondary attacks of diphtheria occurred in people who had previously had the disease, and these became far more common.
Immunisation became worldwide policy after the 1939-1945 war with the death and incidence trend continuing to fall, until the disease appeared to have almost vanished by 1985.
While the latest textbook, Pathology of Infectious Diseases, 1997, is at least more honest, the majority of doctors consider that the elimination of diphtheria is due to the use of toxin-antitoxin and vaccination. The New Zealand Health Department has also adopted this predictable approach. Diphtheria, however, is not a simple disease. In my opinion, not only did the use of the vaccine have little to do with the eradication of diphtheria, but vaccinations and the blanket use of antibiotics have set the world up for a catastrophe of unprecedented proportions. My reasons for this are as follows: -
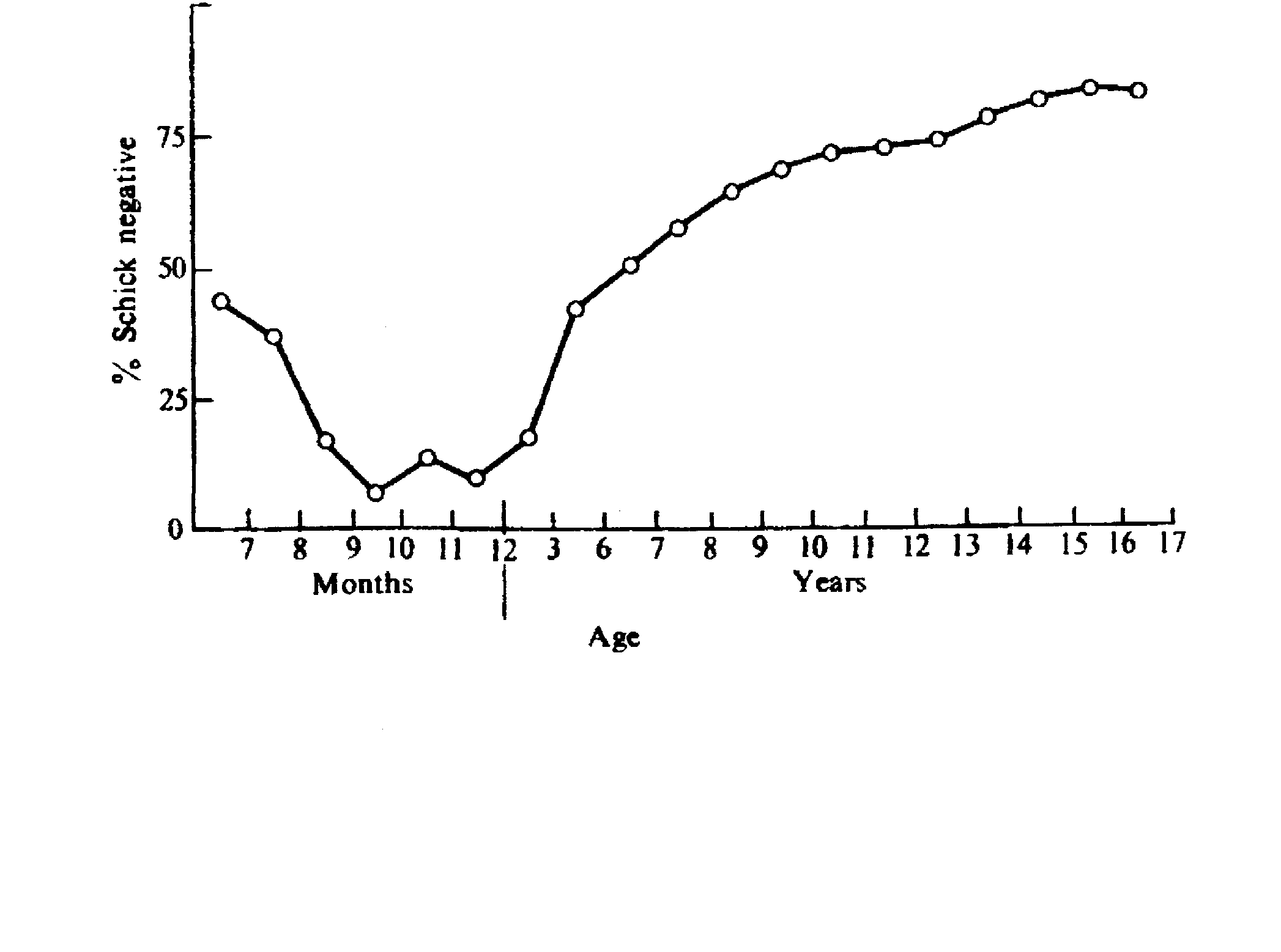
"When diphtheria was prevalent in a city in the days before immunization it was usual to find 2–5 per cent of apparently healthy children with bacilli in their throats at any one time. Since, on average each individual could be demonstrated to carry the organism for no more than a few weeks it can be calculated that most of them must have been re-infected on numerous occasions throughout childhood. Yet even in those days not more than 5–10 per cent of children ever suffered from clinical diphtheria, so that we can feel sure that on most occasions the presence of diphtheria bacilli in the throat did not produce the disease. Thereafter the process of active immunization proceeded as a result of casual, usually non-symptomatic infection by diphtheria bacilli and most children had acquired immunity before they reached their teens." (Burnet, 1972, p. 196).

The development of immunity to diphtheria during childhood, shown as the percentage of children at various ages who are Schick negative, i.e. immune to diphtheria. The immunity of infants is derived passively from their mothers, and disappears during the first year of life. After that time immunity is acquired as a result of infections, which are usually subclinical. (Burnet, 1972 p. 194).
Why the increase in adults contracting diphtheria? I believe this trend was as a result of two early medical practices:
a) The routine use of antitoxin, and later antibiotics, for all contacts as well as cases,
b) The routine use of antibiotics for all sore throats, many of which would have been diphtheria and so would have led to the subclinical development of natural immunity
By preventing diphtheria related subclinical sore throats, you prevent the natural circulation of bacteria in the community, and you also prevent individuals either developing immunity to, or boosting previously acquired immunity to, diphtheria.
The literature makes two things quite clear. Protection from antitoxin was transient, and within 6 – 8 weeks the person would again become susceptible. Antitoxin used as treatment would make it highly unlikely that the patient would activate natural development of disease induced antitoxin; and:
"Early therapy of diphtheria with antibiotics may lead to recurrence of the disease if exposure to fresh infections occurs shortly after discontinuation of treatment, suggesting that the development of antitoxic immunity is suppressed in these cases." (Harrison, 1977, p. 878).
In other words, both injected antitoxin and antibiotics de-rail the immune system, and prevent development of natural immunity.
Furthermore, older textbooks used to note that second attacks of diphtheria were rare, and that even though 10 percent of patients who had had the disease remained Schick-positive they rarely got a second attack. "This suggests that factors other than antitoxin may play a role in protection against infection." (Harrison, 1977, p. 878).
The myth that vaccination is the primary factor that eliminated diphtheria worldwide is highlighted by the evolving situation in Russia (and other countries) today. Graphs of diphtheria from any country show what are called "epidemic cycles". The latest Russian cycle is the normal duration for cycles seen pre-vaccination era; so to say that vaccination has stopped diphtheria in Russia is highly debatable. The Lancet (1996) reported that in 1995 the Ukraine had re-vaccinated the entire population and that diphtheria continued unabated. The vaccine was tested and found to be fine.
Medical literature has always recognised that social and economic dislocation has been the primary friend of diphtheria, along with other diseases. Literature published before the dissolution of stability in Russia makes that clear:
"A serious dislocation of the economy or society of the United States might well increase the incidence of diphtheria as well as other infectious diseases." (Biol. and Clinic. Basis of Infect.Dis, 1985, pg. 230).
The questions raised in the most recent editorial of Eurosurveillance need far more careful thought than accepting the answer that repeated re-vaccination will cure all the problems:
"Why has the resurgence in cases in the Newly Independent States been predominantly in adults if the profound decrease in immunisation levels mainly affected children? What special conditions contributed to the increased vulnerability of the adult population in Russia? Does prevention depend upon frequent boosting immunisations for adults? If the answer is yes, then why hasn't an epidemic occurred in Western Europe? Opportunities for diphtheria transmission must have increased in the East due to declining social conditions and population migration, but why this should have exploited waning adult immunity so rapidly is unclear. Has a change in antibiotic usage as a secondary effect of economic transition allowed diphtheria to flourish?"
I believe that these "experts" are not able to properly answer these questions because they do not understand the history of diphtheria, the real nature of infectious diphtheria, the issues of host resistance, or the role of both antitoxin and antibiotics in preventing the development of immunity to diphtheria. These are the keys to understanding why Russia has experienced such a resurgence of diphtheria.
DECLINE OF DIPHTHERIA IN DEVELOPED COUNTRIES
The most recent textbook states (Pathology 1997 p. 534):
"The dramatically changing incidence of diphtheria during the past decades in developed countries is at least partially the result of widespread childhood immunization although a full explanation is not clear." (Pathology 1997 p. 534)
It is my opinion that the decline of diphtheria in developed countries (including New Zealand) is directly correlated to poverty, social conditions, nutrition, sanitation etc.
Those who know the nutritional history of Europe and Great Britain will recall the many campaigns against such things as rickets. In 1933, 30+ of children who attended one English well-to-do toddlers' clinic were definitely rachitic (Lancet, May 18, 1933, pg. 1189.). The Lancet also reported on February 2nd of that year, that rickets could be detected in not less than 50+ of those who attended infant welfare centres countrywide. And this was supposedly an improvement! Diphtheria and other diseases rose and fell in direct relation to housing, nutritional improvement and wartime conditions, a factor taken into little account by those who consider vaccination to be the only relevant sacrament. The return of conditions of social dislocation and poverty will see an increase in all diseases which, under times of duress, have no respect for the vaccination status of anyone.
The clinical presentation of diphtheria can be divided into two major types – respiratory tract and extra respiratory infections. Clinical manifestations of respiratory tract disease are variable and depend on three things:
The incubation period varies from 2 to 4 days, with older textbooks stating 1 to 7 days.
The medical literature makes it quite clear that host factors are involved:
"…underlying disease, particularly alcoholism, predisposes to more serious manifestations of diphtheria" (JAMA, 1974, p. 1892).
This article also says that vaccination does not prevent carriage of diphtheria, nor prevent clinical disease. The authors studied cases and deaths from 1959-1970 in the USA and state:
"Ten per cent of the cases studied were in persons with full immunization; although this finding may indicate a need for redefinition of this category, it also emphasises that diphtheria can and does occur in persons who have received diphtheria toxoid."
Presumably, host factors also influence why vaccinated people still get diphtheria, just as they influence how severely people will get it naturally.
FAUCIAL diphtheria is the most common clinical presentation, and involves the mouth, tonsil and pharynx. While symptoms may vary, the infection starts quite suddenly with a sore throat, mild throat infection, tiredness and a low temperature. The tonsil and the back of the throat can show a green/yellow exudate that can change to a white glossy pseudomembrane. This can be removed easily. It can then change to a grey colour, with areas of green or black. This membrane cannot be removed without causing bleeding. The neck glands swell and become tender; resulting in the "bull-neck" appearance most commonly associated with mumps. Quite often there will be laryngeal involvement that sometimes shows up before the throat involvement. Initial symptoms are hoarseness, cough, rattly breathing or dyspnoea (difficulty breathing). A membrane in the bronchials can further complicate reanimation, and the risk of suffocation is high without immediate medical intervention.
Growth of the organism is superficial in most cases, and there is little tendency to invade the lymphatic system or bloodstream, except in the terminal stages. The problem is the effects of the toxin produced by the B phage, which can be absorbed and carried by the blood to all parts of the body. The toxic effects are greatest when the primary infection is in the pharynx, less when it is in the larynx and least when it is on the nasal mucosa or skin. If infection involves all the respiratory areas and throat, the level of poison can be extreme.
TREATMENT OF DIPHTHERIA – NOW AND IN HISTORY,
Today, there are only two treatments likely to be given to diphtheria sufferers:
However, an understanding of historical treatments, and other treatments that you may never have heard of, can be useful. Before 1928, one of the most common treatments along side antitoxin was alcohol.
The Lancet, 1928, p. 516 stated:
"Alcohol, which for long has been regarded as indispensable in diphtheria, so far from being of any value in the disease, is liable to increase the myocardial degeneration initiated by the diphtherial poison. In 1927, when no alcohol at all was used in the treatment at the Western Hospital, the case mortality (3.01 per cent) was lower than in any of the other M.A.B. hospitals."
These days, no one in his or her right mind would give alcohol to anyone with a toxin-mediated disease. This has been shown by the 25.7%, diphtheria death rate in Russian alcoholics. But in those days, every medical treatment, including vaccine usage, was solely empirical i.e. based on personal opinion. For example, in 1935 various drug treatments were promoted, and stated to be extremely valuable, but are not considered today. Some extracts from a medical article read:
"Every case of diphtheria is put on to a mixture of digitalis and squills [another valuable and much ignored heart stimulant], and also given calcium by mouth or intramuscularly...with the sudden onset of signs of cardiac arrest camphor, given in oil intramuscularly, acts like a charm. In regard to toxaemia the solution is the administration of pituitrin...since the institution of this procedure early last year there has been an almost complete absence of those cases which simply fade away with sunken grey faces, no pulse and the appearance one associated with extreme shock. Brandy too is valuable both by mouth and intramuscularly. Post diphtheritic paralysis is difficult to treat...port wine and other such stimulants, even in children, give apparently valuable results." (BMJ, 1935, p. 852). [There is a related but unquoted article in BMJ, April 6th, 1935, p. 711].
None of these treatments are even considered now. Neither is homeopathy, which was empirically used with such success by many U.K. and U.S. doctors (in the days before medical association determined what you thought and did), and scoffed at by the establishment, nor the most important treatment of all – Vitamin C. Yet the medical information on this compound is vast, and totally ignored. Why? Because it was done in the early 30's, and natural compounds are not patentable.
Four separate studies done in 1934, 1935, and 1937, found that Vitamin C had the power to neutralise, inactivate and render harmless diphtheria toxins.
In 1934, the unusual resistance of the mouse to diphtheria infections was attributed to its ability to synthesize rapidly its own ascorbic acid, while the guinea pig's ready susceptibility to the disease (like man's) was attributed to its inability to replenish its store of ascorbic acid. Not one of these revelations was even considered by the medical hierarchy, even though yet another study in the Lancet (1937) reported that:
"Infected patients appear to be in a condition of relative "unsaturation" with respect to the vitamin."
And that
"…diphtheria toxin, which, as is well known, causes extensive injury to the supra-renal glands, at the same time brings about a diminution in their vitamin C content. Apart from these investigations, little methodical work on the influence of toxins on the vitamin-C content of the body tissues seems to have been hitherto attempted."
However, they did note that "…the infections cause the disappearance of a considerable proportion of Vitamin C reserves, whether they were high or low, and not merely of a fixed arithmetical difference". No consideration was given to the therapeutical benefits of replacing Vitamin C, or using it as the known antitoxin it had already proved to be. It appears that at this point, the medical hierarchy put a stop to any further related research.
Following this work, there were huge numbers of studies done on Vitamin C, with all of them using Vitamin C only in the context of a Vitamin, rather than therapeutically as an "antibiotic". Trials of megadoses were discouraged, especially when funded by pharmaceutical companies who could neither patent, nor make money out of it. However, many doctors used vitamin C for treating all toxin-mediated diseases, as per the original research, with very successful results that they could only report in the lay press. Except for one of the most outspoken ones, Dr Fred Klenner. Dr Klenner got much of his research and case studies published in the Tri-State Medical Journal in U.S.A (and a few others). Having read all the information available on the action and use of Vitamin C, I have no doubt whatsoever that Vitamin C could treat diphtheria far more successfully than antitoxin, and without the huge risks that come with a foreign product made in horses. I also believe it would allow the development of naturally induced immunity.
Dr Klenner (1957) made one of the most telling comments when recounting his successes with Vitamin C:
" But then there are some physicians who would stand by and see their patient die rather than use ascorbic acid – because in their finite minds it exists only as a vitamin."Note: Before commencing any treatment we recommend consultation with a registered practitioner.
Diphtheria. (True, malignant, membranous diphtheria)
Mercurius cyanatus 6 – 30, every hour.
At the same time the throat may be cleansed from time to time with a wash of Phytolacca tincture (5 drops to the ounce). A small sponge, fixed in a handle, sold by chemists, being the best means. [A teaspoonful of yeast may be given every two or three hours.] This treatment alone will suffice for the great majority of attacks.
If this does not control it, Echinacea tincture 1 drop 1 – 2 hourly.
When there is oedema of the throat, Apis 3x, every hour.
Excessive pain on swallowing, throat livid, ulcerated, external neck swollen, prostration, Ailanthus 3x, 1hourly.
Air-passages involved, and the croup symptoms becoming worse, Iodum 1, 1hourly.
Great prostration, the constitutional symptoms predominating much over the amount of local affection; beginning on left side and spreading to right, Lachesis 6, 1hourly. When the affection begins on right side and spreads to the left, Lycopodium 6 – 30, hourly. Changing from side to side, Lac. canium 30 – 200, 1 – 2hourly.
When prostration is extreme, Arsenicum 3, every ten minutes, will often restore the patient. The greatest care must be taken not to raise the patient from the recumbent position, as that is often of itself sufficient to induce fatal syncope.
Scarlatinal Diphtheria.
The treatment in general is the same as above. If, however, there is much swelling in the external glands, Mercurius biniodatus 3x, 2hourly can be given. The throat can be cleansed, if necessary, with Phytolacca gargle as above.
Feverish Diphtheria.
With high fever, pains in the back and limbs, but no prostration, Phytolacca 1x, 1hourly, with the local application of Phytolacca tincture as above.
After Effects.
Weakness: Psorinum 30, 4hourly.
Paralysis: Gelsemium 1, 3hourly.
Paralysis of vocal cords or bladder: Causticum 30, 2 – 4hourly.
Deafness: Muriaticum acidum 1, 2hourly.
Make a mixture of the following:
To soothe inflamed throat – Slippery Elm and/or Marshmallow.
To cleanse – Horehound or Sage.
To purify blood – Golden Seal and/or Echinacea.
To provide extra nourishment – Lemon juice, rind or 1 drop Lemon oil.
Inhalation: Oils of Lemon & Eucalyptus can be used as an inhalation (3
drops into steaming water) or gargle (1-2 drops with a glass of water).
CELL SALTS:
Nat Phos, Ferr Phos and Kali Mur can be given together every two
hours at the first sign of fever, illness and sore throat.
Kali Phos for exhaustion and offensive breath.
Kali Mur and Calc Phos – alternate for difficult breathing.
REFERENCES: -
Beddow-Bayly, M. (1939). The Schick inoculation for immunisation against diphtheria.
The Biological and Clinical Basis of Infectious Diseases. (3rd ed.). (1985). P.
230.
British Medical Journal, April 20, 1935.
Burnet, Sir MacFarlane. (1972). Natural history of infectious disease.
Emerging Infectious Diseases. Vol. 4 No. 4 October/December 1998.CDC, Atlanta.
Eurosurveillance. Vol. 2 No. 8/9.
Harrison’s Principles of Internal Medicine (8th ed.). Vol. I, 1977.
Journal of the American Medical Association, March 4th, 1922.
Journal of the American Medical Association, Vol. 229, No. 14. September 1974.
Klenner, Fred R. (1957). The black widow spider. Tri-State Medical Journal. December 1957.
The Lancet, September 8, 1928.
The Lancet, July 24, 1937.
Maclean, F. S. (1964). Challenge for Health – a history of public health in New
Zealand. Wellington: Govt. Print.
Medical World, February 6th, 1931.
Mortality and Morbidity Weekly Report. March 17, 1995.
Pathology of Infectious Diseases. (1997).
Scandinavian Journal of Infectious Diseases. Vol. 28, 1996, p. 41-46.
Vitek, Charles R and Melinda Wharton. (unknown). Diphtheria in the former Soviet Union – re-emergence of a pandemic disease.
WHO meeting July 1993. EUR/ICP/EPI 038 Rev 1.